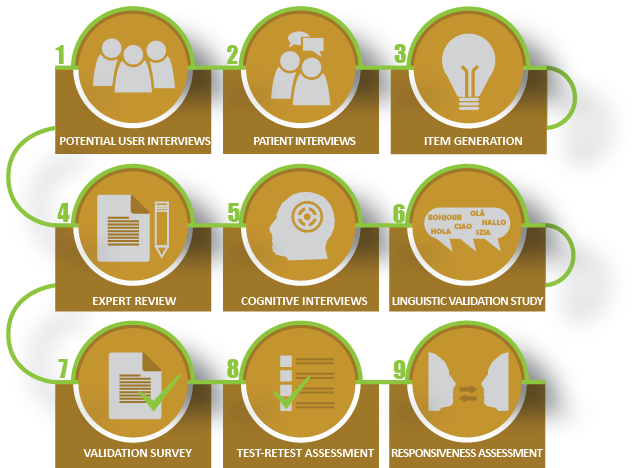
The primary use of the Ox-PAQ is intended to be in clinical trials and related forms of evaluation of interventions targeted at maintaining activity and participation. The latest progress on the instrument’s development and validation can be viewed at the University of Oxford Health Services Research Unit website:
https://www.ndph.ox.ac.uk/research/health-services-research-unit-hsru/research/oxpaq-initiative
Validated Populations
- Aneurysmal subarachnoid hemorrhage
- Chronic obstructive pulmonary disease
- Motor neurone disease
- Multiple sclerosis
- Parkinson’s disease
- Valvular heart disease
^ Back to top